Every year, over a million people in the U.S. end up in the emergency room because of unexpected reactions between their medications. Many of these cases could have been avoided with a simple conversation with a pharmacist. You might think your doctor handles all the safety checks, but the truth is, your pharmacist is the one who sees the full picture - every pill, every supplement, every juice you drink, and every health condition you have. And they’re trained to catch what others miss.
Why Drug Interactions Matter More Than You Think
A drug interaction happens when something changes how a medicine works in your body. It might make it weaker, stronger, or cause side effects you never expected. These aren’t rare glitches. They’re common. The FDA says over 112,000 emergency visits in 2022 were directly linked to drug interactions. The biggest culprits? Blood thinners like warfarin, diabetes drugs, heart medications, and painkillers. But here’s the twist: you don’t need to be on five drugs to be at risk. Sometimes, just one new supplement or a daily glass of grapefruit juice is all it takes.Interactions fall into three main types:
- Drug-drug: When two or more medications react - like taking aspirin with warfarin and increasing bleeding risk.
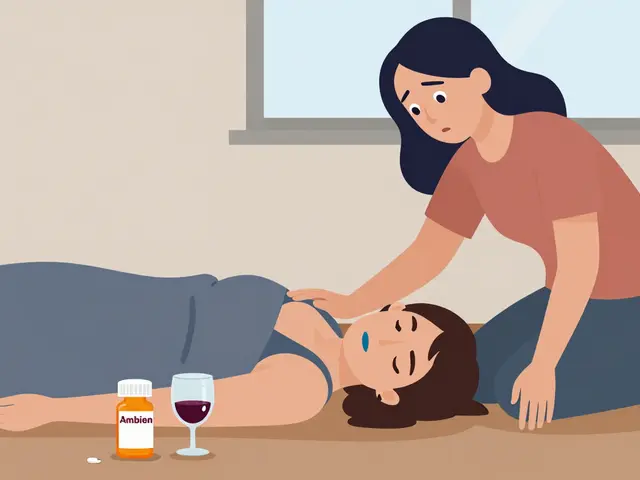
- Drug-food/beverage: Grapefruit juice can block how your body breaks down statins, causing dangerous buildup. Alcohol can make sedatives too strong. Even high-sodium foods can interfere with blood pressure meds.
- Drug-condition: If you have kidney disease, some drugs can’t be cleared properly. If you have high blood pressure, decongestants in cold meds can spike your pressure dangerously.
And here’s the thing most people don’t realize: over-the-counter meds, vitamins, and herbal supplements are just as risky as prescription drugs. St. John’s wort can make birth control fail. Calcium supplements can block thyroid meds. Turmeric might thin your blood. If you’re taking anything outside a prescription bottle, it still counts.
What to Ask Your Pharmacist - The 7 Must-Ask Questions
You don’t need to be a medical expert to protect yourself. Just ask these seven questions every time you pick up a new prescription or refill - and don’t stop until you get clear answers.- Can this medicine interact with any of my other medications? Don’t just list your prescriptions. Include everything: the ibuprofen you take for your back, the melatonin for sleep, the fish oil, the ginseng, even the antacid you use daily. Pharmacists use systems that check for over 10,000 possible interactions. But they can’t do it if you leave something out.
- Should I avoid certain foods, drinks, or supplements while taking this? Grapefruit juice is the most famous offender - it messes with over 85 medications, including some statins, blood pressure drugs, and anti-anxiety pills. But it’s not just grapefruit. Alcohol, caffeine, high-salt diets, and even dairy can change how your body handles meds. Ask specifically about your daily habits.
- How will this affect my existing health conditions? If you have diabetes, liver disease, kidney issues, or heart problems, some drugs can make them worse. For example, decongestants in cold medicines can raise blood pressure. Antihistamines can worsen glaucoma. Tell your pharmacist your full medical history - even if you think it’s unrelated.
- What are the warning signs of an interaction? You need to know what to watch for. Dizziness, nausea, irregular heartbeat, unusual bruising, confusion, or sudden fatigue could mean something’s off. Ask for the top three red flags specific to your meds.
- When and how should I take this? With food? On an empty stomach? At a certain time of day? Timing matters. Some drugs need to be taken 2 hours before or after other meds. Others work better with food. Calcium supplements can block antibiotics if taken together. Even small timing changes can prevent serious issues.
- Is there a safer alternative if this interacts badly? Sometimes, there’s another drug that does the same job without the risk. Ask if there’s a different option that’s less likely to clash with your current regimen.
- Do I need to update my list every time something changes? Yes. The most common cause of interactions? A new medication added without a full review. Pharmacists recommend updating your medication list every 3 months - or every time you see a new doctor. Keep it simple: name, dose, frequency, and why you’re taking it.
What to Bring to Your Pharmacist Visit
Don’t rely on memory. Bring a written list. Include:- All prescription medications (including dosages and how often you take them)
- All over-the-counter pills - pain relievers, antacids, sleep aids
- All vitamins, minerals, and herbal supplements
- All topical products - creams, patches, eye drops (yes, even these can interact)
- Any alcohol or recreational drug use
- Your typical diet - especially if you drink grapefruit juice, eat a lot of leafy greens, or consume high-sodium foods daily
Many people think their doctor knows all this. But doctors see you for 10 minutes. Pharmacists see you every time you refill. They’re the ones who track patterns over months. The more complete your list, the better they can protect you.
Why Supplements Are the Hidden Risk
Seventy-seven percent of American adults take at least one supplement. Most think they’re harmless. But supplements aren’t regulated like drugs. That means no one checks how they interact with your prescriptions. St. John’s wort, for example, can reduce the effectiveness of antidepressants, birth control, and even HIV meds. Garlic supplements can thin your blood - dangerous if you’re on warfarin. Echinacea can interfere with liver enzymes that break down drugs. Vitamin K can undo the effects of blood thinners. And you won’t find any warning labels on the bottle.Always ask: "Is this supplement safe with my current meds?" Even if it’s "natural," it’s still a chemical that affects your body. Your pharmacist has access to databases that track these hidden risks. Use them.
How Pharmacies Are Fighting Back
Pharmacies today aren’t just handing out pills. CVS, Walgreens, and others use real-time systems that scan your full medication history when you fill a new prescription. These systems flag over 90% of common interactions. But they still miss about 18% - because they only see what’s in their system. If you took a supplement last week and didn’t tell them, it won’t show up.Pharmacists are also trained to ask about social factors: Do you have trouble affording meds? Do you forget doses? Are you taking meds from different doctors? These things increase interaction risk. The American Society of Health-System Pharmacists now trains pharmacists to look at the whole person - not just the pills.
What Happens If You Don’t Ask?
The consequences aren’t theoretical. A 72-year-old man in Florida took simvastatin for cholesterol and started drinking grapefruit juice daily. He didn’t think it mattered. He ended up in the hospital with muscle damage so severe he needed surgery. A woman in Texas took ibuprofen with her blood pressure med for headaches. Her kidneys started failing. Both cases were preventable.Drug interactions don’t always cause immediate reactions. Sometimes, damage builds slowly - liver strain, kidney stress, or unstable blood sugar. By the time symptoms show up, it’s too late.
When to Talk to Your Pharmacist
Don’t wait for a problem. Talk to them:- When you get a new prescription
- When you start a new supplement
- When you switch pharmacies
- Every 3 months - even if nothing changed
- After a hospital visit or doctor’s appointment
And if you’re unsure? Call them. Most pharmacies offer free 10-minute consultations. No appointment needed. Just walk in or call. Ask the same seven questions. You’re not bothering them - you’re doing your job.
Final Thought: You’re the Most Important Link
Doctors, pharmacists, and nurses all do their part. But the system only works if you speak up. You’re the only one who knows what you’re really taking - the tea you drink every morning, the gummy vitamins you forgot to mention, the painkiller you took last weekend. Your pharmacist can’t read your mind. But if you give them the full picture, they can keep you safe.Can I just rely on my doctor to check for drug interactions?
No. Doctors focus on diagnosing and treating your condition, but they often don’t have time to review every single medication you’re taking - especially supplements and over-the-counter drugs. Pharmacists are trained specifically to catch interactions. They see your full medication history every time you refill a prescription. They’re your best line of defense.
Are herbal supplements really risky with prescription drugs?
Yes. Supplements like St. John’s wort, garlic, ginkgo, and turmeric can interfere with how your body processes medications. St. John’s wort can make birth control, antidepressants, and HIV drugs stop working. Garlic and ginkgo can increase bleeding risk when taken with blood thinners. These aren’t myths - they’re documented, dangerous interactions. Always tell your pharmacist about every supplement.
What if I forget to mention a supplement I’m taking?
It’s common - and dangerous. Studies show that up to 60% of patients don’t tell their pharmacist about all the supplements they use. Even if you think it’s "just a vitamin," it could be causing a hidden interaction. If you realize later you missed something, call your pharmacy right away. It’s better to admit a mistake than risk a reaction.
Is grapefruit juice really that dangerous?
Yes. Grapefruit juice blocks an enzyme in your gut and liver that breaks down many drugs. This causes the drug to build up to toxic levels. It can affect statins, blood pressure meds, anti-anxiety drugs, and even some cancer treatments. One glass can cause effects that last over 24 hours. If you’re on any prescription, ask if grapefruit is safe - even if you only drink it once a week.
Do I need to update my medication list every time I change something?
Absolutely. The most common cause of drug interactions is a new medication added without a full review. Even a single new pill - like a painkiller or sleep aid - can trigger a reaction. Keep a written list and update it every time you start, stop, or change a medication. Bring it to every pharmacy visit. It’s the simplest way to stay safe.
Can pharmacies tell if my medications are interacting before I even take them?
Yes - if they have your full list. Modern pharmacy systems scan your prescriptions and OTC meds in real time and flag high-risk interactions. But they can’t see what you don’t tell them. If you leave out a supplement, a herbal tea, or an occasional alcohol drink, the system won’t catch it. Your honesty is the key to the system working.
Are older adults more at risk for drug interactions?
Yes. Nearly half of adults over 65 take five or more medications daily. With age, kidneys and liver process drugs slower, so even small interactions can become serious. Plus, older adults often see multiple doctors, increasing the chance of overlapping prescriptions. That’s why pharmacists recommend a full medication review at least twice a year for seniors.